En moyenne, les études scientifiques suggèrent qu’une consommation importante de viande, principalement de viande rouge et de viandes transformées, pourrait être négatif pour la santé, sur la base d’études observationnelles. Ce genre d’études pouvant être entachées de biais, de facteurs de confusion, il est possible que d’autres facteurs que la viande puissent causer ces résultats.
Par exemple, le fait que dans certains pays la viande soit consommée largement sous forme de burgers, et donc accompagnée de produits transformés contenant de fortes doses de glucides pourrait être un facteur de confusion. On pourrait s’attendre alors à ce qu’on trouve des différences avec des pays où la viande est plus souvent consommée avec des légumes et des féculents non transformés. C’est effectivement ce que l’on trouve.
Quelques études ont par ailleurs été menées mesurant les associations entre viande et santé en comparaison d’autres variables. Elles suggèrent un rôle de la viande interagissant avec celui des produits transformés ou des fruits et légumes.
Publications suggérant la faiblesse des preuves contre la viande rouge
Processed meat intake and incidence of colorectal cancer: a systematic review and meta-analysis of prospective observational studies [Abstract]
Händel et al.
European journal of clinical nutrition, 2020
The overall judgment showed that two out of 29 studies had a moderate risk of bias, 25 had a serious risk of bias, and 2 had a critical risk of bias. The bias domains most often rated critical were bias due to risk of confounding, bias due to missing data, and selective outcome reporting bias. Although this meta-analysis indicates a modest association between processed meat intake and an increased risk of CRC, our assessment of internal validity warrants a cautious interpretation of these results, as most of the included studies were judged to have serious or critical risks of bias.
–
Reduction of Red and Processed Meat Intake and Cancer Mortality and Incidence – A Systematic Review and Meta-analysis of Cohort Studies
Han et al.
Annals of internal medicine, 2019
https://www.acpjournals.org/doi/10.7326/M19-0699
The possible absolute effects of red and processed meat consumption on cancer mortality and incidence are very small, and the certainty of evidence is low to very low.
–
Patterns of Red and Processed Meat Consumption and Risk for Cardiometabolic and Cancer Outcome
A Systematic Review and Meta-analysis of Cohort Studies
Vernooij et al.
Annals of internal medicine, 2019
https://www.acpjournals.org/doi/10.7326/M19-1583
Low- or very-low-certainty evidence suggests that dietary patterns with less red and processed meat intake may result in very small reductions in adverse cardiometabolic and cancer outcomes.
–
Red and Processed Meat Consumption and Risk for All-Cause Mortality and Cardiometabolic Outcome
A Systematic Review and Meta-analysis of Cohort Studies
Zeraatkar et al.
Annals of internal medicine, 2019
https://www.acpjournals.org/doi/10.7326/M19-0655
The magnitude of association between red and processed meat consumption and all-cause mortality and adverse cardiometabolic outcomes is very small, and the evidence is of low certainty.
Consommation de viande rouge au sein d’une alimentation équilibrée
Co-consumption of Vegetables and Fruit, Whole Grains, and Fiber Reduces the Cancer Risk of Red and Processed Meat in a Large Prospective Cohort of Adults from Alberta’s Tomorrow Project
Maximova et al.
Nutrients, 2020
https://www.mdpi.com/2072-6643/12/8/2265
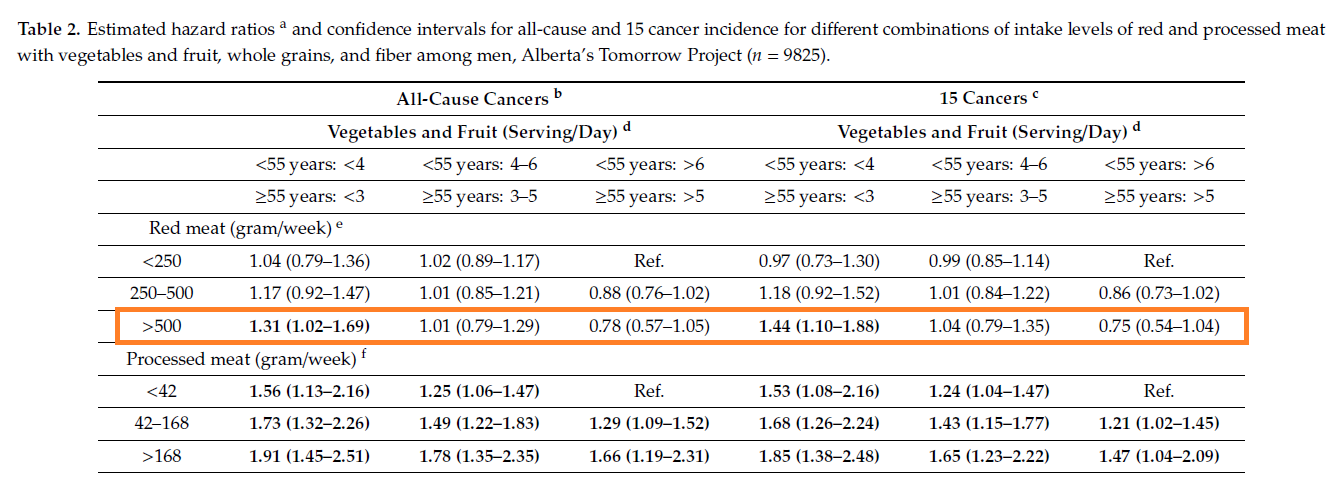
–
Food groups and risk of coronary heart disease, stroke and heart failure: A systematic review and dose-response meta-analysis of prospective studies
Bechthold et al.
Taylor and Francis, 2019
https://www.tandfonline.com/doi/pdf/10.1080/10408398.2017.1392288


Overall, 123 reports were included in the meta-analyses. An inverse association was present forwhole grains (RRCHD: 0.95 (95% CI: 0.92–0.98), RRHF: 0.96 (0.95–0.97)), vegetables and fruits (RRCHD: 0.97(0.96–0.99), and 0.94 (0.90–0.97); RRstroke: 0.92 (0.86–0.98), and 0.90 (0.84–0.97)), nuts (RRCHD: 0.67 (0.43–1.05)), andfish consumption (RRCHD: 0.88 (0.79–0.99), RRstroke: 0.86 (0.75–0.99), and RRHF: 0.80 (0.67–0.95)),while a positive association was present for egg (RRHF: 1.16 (1.03–1.31)), red meat (RRCHD: 1.15 (1.08–1.23),RRstroke: 1.12 (1.06–1.17), RRHF: 1.08 (1.02–1.14)), processed meat (RRCHD: 1.27 (1.09–1.49), RRstroke: 1.17(1.02–1.34), RRHF: 1.12 (1.05–1.19)), and SSB consumption (RRCHD: 1.17 (1.11–1.23), RRstroke: 1.07 (1.02–1.12),RRHF: 1.08 (1.05–1.12)) in the linear dose-response meta-analysis. There were clear indications for non-linear dose-response relationships between whole grains, fruits, nuts, dairy, and red meat and CHD.Conclusion: An optimal intake of whole grains, vegetables, fruits, nuts, legumes, dairy,fish, red andprocessed meat, eggs and SSB showed an important lower risk of CHD, stroke, and HF.
–
A Mediterranean-style eating pattern with lean, unprocessed red meat has cardiometabolic benefits for adults who are overweight or obese in a randomized, crossover, controlled feeding trial [Texte]
O’Connor et al.
American journal of clinical nutrition, 2018
Adults who are overweight or moderately obese may improve multiple cardiometabolic disease risk factors by adopting a Mediterranean-style eating pattern with or without reductions in red meat intake when red meats are lean and unprocessed.
–
Vegetarian diet, Seventh Day Adventists and risk of cardiovascular mortality: A systematic review and meta-analysis
Kwok et al.
International journal of cardiology, 2014
https://www.internationaljournalofcardiology.com/article/S0167-5273(14)01290-X/fulltext
Vegetarian diet is potentially associated with reduced ischaemic heart disease.The benefits of a vegetarian diet are most apparent among Seventh-Day Adventist.Reductions in all-cause mortality were not replicated in the non-Adventist studies.Evidence supporting a vegetarian diet is driven by Seventh-Day Adventists studies.The effect of vegetarian diet in other non-Adventist cohorts remains unproven.
Is Grassfed Meat and Dairy Better for
Human and Environmental Health?
Provenza et al.
Frontiers in nutritions, 2019
Méta-analyses sur la viande
Association between red meat consumption and colon cancer:
A systematic review of experimental results
Turner & Lloyd
Experimental biology and medicine, 2017
Forty studies using animal models or cell cultures met specified inclusion criteria, most of which were designed to examine the role of heme iron or heterocyclic amines in relation to colon carcinogenesis. Most studies used levels of meat or meat components well in excess of those found in human diets. Although many of the experiments used semi-purified diets designed to mimic the nutrient loads in current westernized diets, most did not include potential biologically active protective compounds present in whole foods. Because of these limitations in the existing literature, there is currently insufficient evidence to confirm a mechanistic link between the intake of red meat as part of a healthy dietary pattern and colorectal cancer risk.
–
Health risk factors associated with meat, fruit and vegetable consumption in cohort studies: A comprehensive meta-analysis
Grosso et al.
PlosOne 2017
https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0183787
Another important confounding factor/effect modifier may be related to cultural and geographical aspects, as suggested by the stronger association between meat consumption and colorectal cancer risk in US than European studies [123].
–
Food groups and risk of all-cause mortality: a systematic review and meta-analysis of prospective studies
Schwingshackl et al.
The american journal of clinical nutrition, 2017
https://academic.oup.com/ajcn/article/105/6/1462/4569801
With increasing intake (for each daily serving) of whole grains (RR: 0.92; 95% CI: 0.89, 0.95), vegetables (RR: 0.96; 95% CI: 0.95, 0.98), fruits (RR: 0.94; 95% CI: 0.92, 0.97), nuts (RR: 0.76; 95% CI: 0.69, 0.84), and fish (RR: 0.93; 95% CI: 0.88, 0.98), the risk of all-cause mortality decreased; higher intake of red meat (RR: 1.10; 95% CI: 1.04, 1.18) and processed meat (RR: 1.23; 95% CI: 1.12, 1.36) was associated with an increased risk of all-cause mortality in a linear dose-response meta-analysis.
[…] Each additional daily 100 g of red meat was positively associated with risk of all-cause mortality (RR: 1.10; 95% CI: 1.04, 1.18; I2 = 92%; P-heterogeneity < 0.001; n = 10)
[…] Analyses of the EPIC (European Prospective Investigation into Cancer and Nutrition) cohort showed a slight J-shaped positive association between red meat consumption and all-cause mortality; the lowest risk was identified among participants with low to moderate meat consumption (120).
–
Potential health hazards of eating red meat
A. Wolk
Journal of internal medicine, 2016
https://onlinelibrary.wiley.com/doi/full/10.1111/joim.12543
High unprocessed red meat consumption was not significantly associated with the increased all‐cause mortality (RRsummary 1.10, 95% CI 0.98–1.22 for the highest versus the lowest category of consumption). In a dose–response meta‐analysis, an increase in the consumption of unprocessed red meat of 100 g day−1 was associated with a borderline statistically significant 9% increased risk (RRsummary 1.09, 95% CI 0.997–1.20); heterogeneity between studies was observed. In a recent meta‐analysis, the authors identified the source of the between‐study heterogeneity 78. For the US populations (four cohorts), a dose–response analysis showed that each serving per day of unprocessed red meat consumption was positively and statistically significantly associated with risk of all‐cause mortality (RRsummary 1.15, 95% CI 1.12–1.19; no heterogeneity); summaries of results from European and Asian cohorts did not show positive associations.
–
Red and processed meat consumption and mortality: dose–response meta-analysis of prospective cohort studies
Wang et al.
Public health nutrition, 2015
https://dash.harvard.edu/bitstream/handle/1/41426835/84562%20red-and-processed-meat.pdf?sequence=1
There was evidence of a non-linear association between processed meat consumption and risk of all-cause and cardiovascular mortality, but not for cancer mortality. For processed meat, the pooled relative risk with an increase of one serving per day was 1·15 (95 % CI 1·11, 1·19) for all-cause mortality(five studies;P<0·001 for linear trend), 1·15 (95 % CI 1·07, 1·24) for cardiovascular mortality (six studies;P<0·001) and 1·08 (95 % CI 1·06, 1·11) for cancer mortality (five studies;P<0·001). Similar associations were found with total meat intake. The association between unprocessed red meat consumption and mortality risk was found in the US populations, but not in European or Asian populations.
–
Red Meat and Processed Meat Consumption and All-Cause Mortality:
A Meta-Analysis
Larsson et al.
American journal of epidemiology, 2014
https://academic.oup.com/aje/article/179/3/282/103471
In a dose-response meta-analysis, consumption of processedmeat and total red meat, but not unprocessed redmeat, was statistically significantly positively associated with all-cause mortality in a nonlinear fashion.
[…] Unprocessed red meat consumption was positively associated with allcause mortality in studies from the United States (RR = 1.23, 95% CI: 1.17, 1.30; Pheterogeneity = 0.30; n = 3 studies) but not in European studies (RR = 0.90, 95% CI: 0.59, 1.38; Pheterogeneity = 0.002; n = 2 studies).
–
Association between total, processed, red and white meat consumption andall-cause, CVD and IHD mortality: a meta-analysis of cohort studies
Abete et al.
British journal of nutrition, 2014
https://www.cambridge.org/core/services/aop-cambridge-core/content/view/35CB32B716F2FBAF6119070029193544/S000711451400124Xa.pdf/div-class-title-association-between-total-processed-red-and-white-meat-consumption-and-all-cause-cvd-and-ihd-mortality-a-meta-analysis-of-cohort-studies-div.pdf
In the dose– response meta-analysis, an increase of 50 g/d inprocessed meat intake was found to be positively associated with all-cause and CVD mortality, while an increase of 100 g/d in red meatintake was found to be positively associated with CVD mortality. No significant associations were observed between consumption of anytype of meat and IHD mortality. The results of the present meta-analysis indicate that processed meat consumption could increase the riskof mortality from any cause and CVD, while red meat consumption is positively but weakly associated with CVD mortality.
Poisson
Fish consumption and all-cause mortality: a meta-analysis of cohort studies
Zhao et al.
European journal of clinical nutrition, 2016
https://www.nature.com/articles/ejcn201572
Twelve prospective cohort studies with 672 389 participants and 57 641 deaths were included in this meta-analysis. Compared with the lowest category, the highest category of fish intake was associated with about a 6% significantly lower risk of all-cause mortality (RR=0.94, 95% confidence interval (CI): 0.90, 0.98; I2=39.1%, P=0.06). The dose–response analysis indicated a nonlinear relationship between fish consumption and all-cause mortality. Compared with never consumers, consumption of 60 g of fish per day was associated with a 12% reduction (RR=0.88, 95% CI: 0.83, 0.93) in risk of total death.
Vegetarian, vegan diets and multiple health outcomes: A systematic review
with meta-analysis of observational studies
Dinu et al.
Critical reviews in food science and nutrition, 2017
https://www.researchgate.net/publication/293329136_Vegetarian_vegan_diets_and_multiple_health_outcomes_A_systematic_review_with_meta-analysis_of_observational_studies
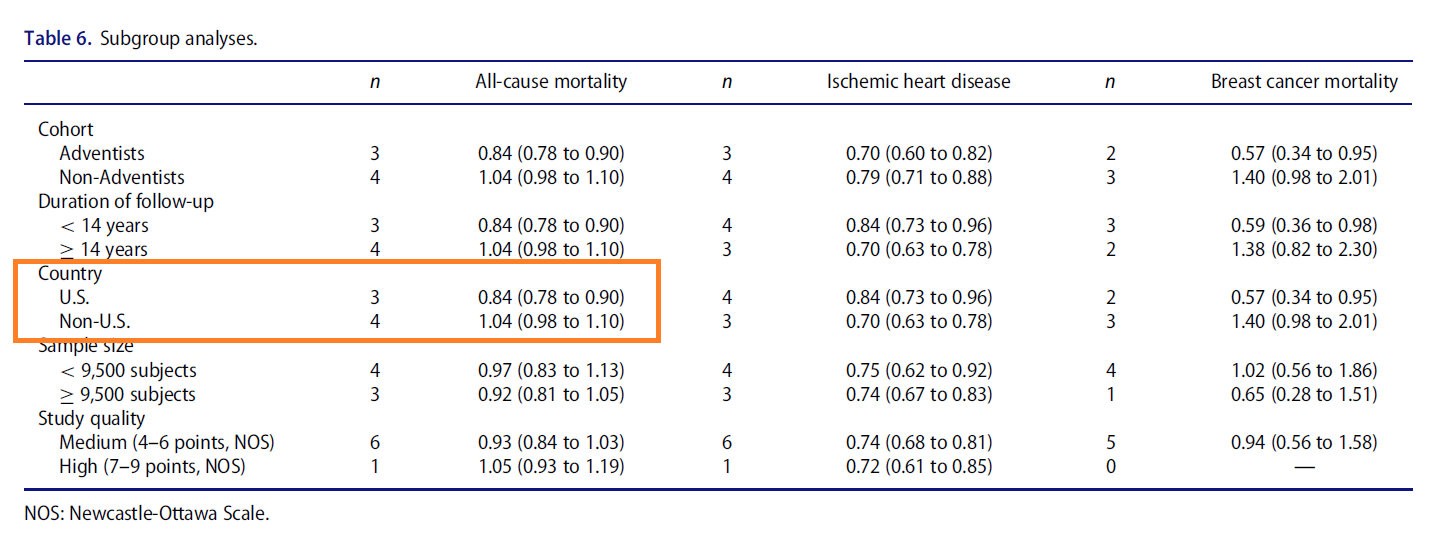
–
Reddit « red meat science » [Page]
